Poor UTI guidelines are driving AMR in women




The partnership between Forte Medical and Owen Mumford USA was launched today at the OCTANe Medical Innovation Technology Forum (MTIF) at Newport Beach, CA 28-29 October 2019. … Read More

A rise in persistent UTIs… Read More

An interesting study published in the Scandinavian Journal of Primary Health Care which concludes: “MSU samples should be used in general practice for optimal accuracy… Read More

Its time to reignite our NHS! Now our beloved health system has been blessed with new funding, we can furnish every hospital and GP practice… Read More

Today’s Hippocratic Post features an overview on the importance of urine and the evidence supporting why our technology plays such a vital role in… Read More

This is the latest recommendation following publication of a Californian study about the rise of antibiotic-resistant bacteria. But right-first-time diagnosis and treatment is only… Read More
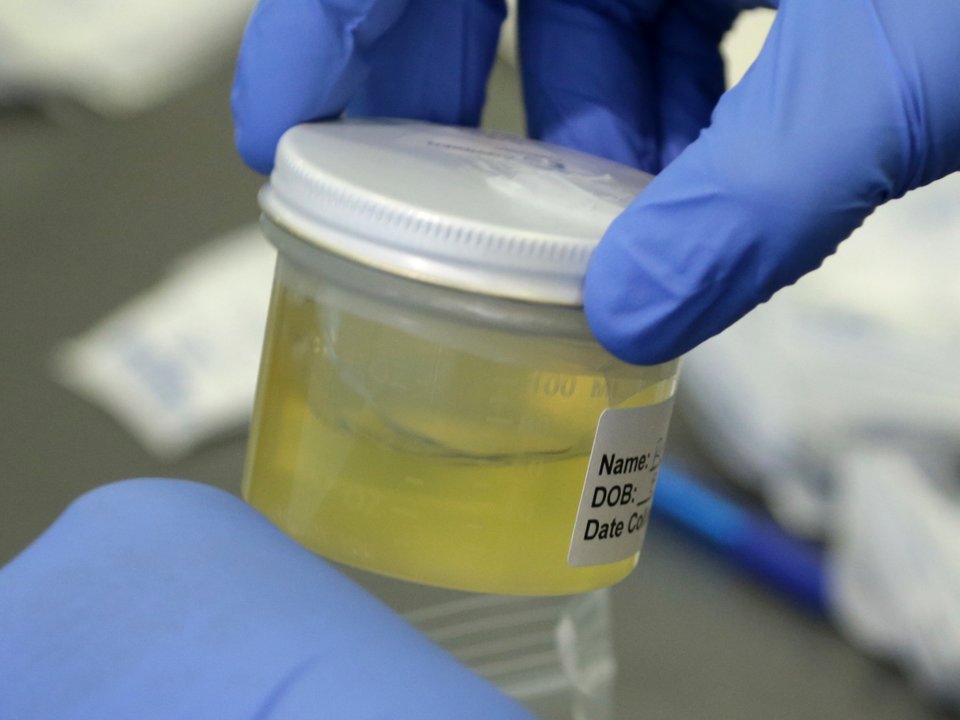
A new study shows that Antibiotic-resistant UTI bacteria is becoming more common; Knowlex has created a short-film about the research and what you should know… Read More
