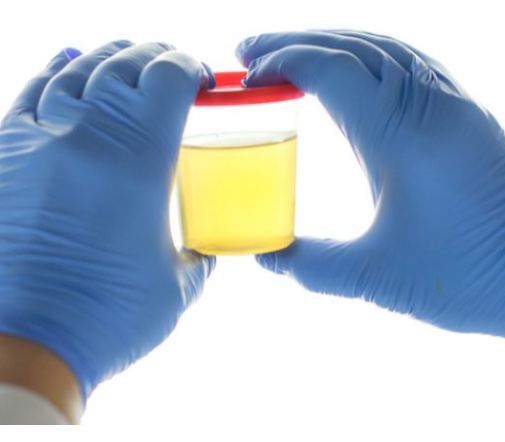
Med-Tech Innovation Expo – April 2018
Giovanna Forte is one of the guest speakers at this two day and her presentation: “Urine Trouble – How Innovation is Transforming Basic Medicine” –… Read More

Giovanna Forte is one of the guest speakers at this two day and her presentation: “Urine Trouble – How Innovation is Transforming Basic Medicine” –… Read More

Despite its importance, there is no standard for urine collection. In this article the author, Professor Frank Chinegwundoh, discusses the problem of inadequate samples and… Read More

Antibiotic resistance in children’s E. coli, a bacteria that is the most common cause of urinary tract infection, is high against many antibiotics commonly prescribed in… Read More
Doctors can tell a lot about your health from your urine sample, if taken properly. Insightful piece by Rob Eley and Michael Sinnott from The… Read More

It costs so little to put it right: “The NHS spent £434 million in 2013/14 on treating184,000 patients in unplanned admissions associated with a UTI. … Read More

Cystitis or urinary tract infection (UTI) is the second most common bacterial infection in the UK and around half of all women will experience at… Read More
Paul Benton, International Director at the ABHI shares our story as to how we entered the US marketplace Appointed sales and distribution partners, dedicated warehouse… Read More

From AMR to UTIs, independent participants at this year’s Forum highlighted the clinical and financial case for a “gold standard” urine specimen collection process that… Read More

As a regular participant of the ABHI Trade Missions to Texas, we are delighted to be part of this exciting development…. The Association of British… Read More

The Hippocratic Post is a widely read blog engine for GPs and other physicians. Our Peezy Midstream technology has been acknowledged as a credible… Read More